
By Bashar Abubakar and Hadiza Mohammed (Lead Writers)
When Nigeria conducted a Joint External Evaluation (JEE) in 2017, there was no way of knowing that the COVID-19 pandemic was just three years away. The whole essence of the JEE is to assess a country’s capacity to respond to public health emergencies, and it could be said that the 2017 JEE gave Nigeria a good idea of its capacity to respond to future disease outbreaks. The mid-term JEE in 2019 enabled an assessment of the progress made since 2017 to strengthen the country’s capacity to prevent, detect and respond to infectious disease outbreaks.
Both evaluations provided a better understanding of Nigeria’s national disease response capacities, and although the government made some initial investment into improving the nation’s health security, the COVID-19 pandemic uncovered the huge gaps in the country’s health security.
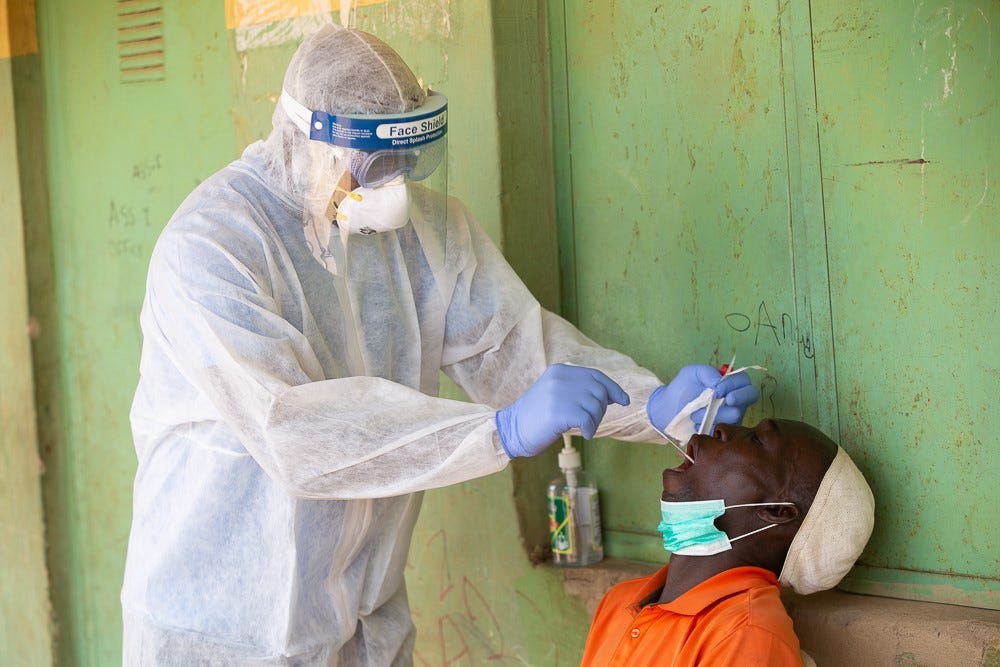
Bridging these health security gaps require engaging with all stakeholders at all levels: national and subnational. The latter, who are usually the first line of defense during public health emergencies, need to be well equipped with the tools necessary for detecting, preventing, and responding to infectious disease outbreaks. This would involve substantial investments in strengthening health systems. It is against this backdrop that the Nigeria Centre for Disease Control (NCDC) revised the national JEE tool so that states could adapt it. Their purpose was to, ultimately, strengthen state systems for disease detection, preparedness, and response.

A state level assessment
Using the adapted JEE tool, with support from the NCDC and partners, Kano State conducted its JEE in June 2021. Fifteen technical areas of infectious disease prevention, detection and response were evaluated, and the state achieved a score of 46%. According to the Preventepidemics.org JEE score ranking, this falls within the ‘Work to Do’ category which suggested that the state needed to do more to strengthen its epidemic preparedness and response (EPR) pillars. Dr. Abdullahi Kauran-Mata, the State Epidemiologist, said that the JEE empowered Kano State to identify and address gaps, which improved its epidemic preparedness and response capabilities.

One of such gaps was the lack of a legal framework for health security in the state. This led to the introduction of the state Public Health Security Bill, which is at the committee level in the State House of Assembly. Dr. Kauran-Mata is confident that once the bill is passed and signed into law, it will improve disease detection and response, and provide dedicated and sustainable budgetary allocation and releases for epidemic preparedness and response in the state. If the bill is signed into law, the ₦300million and ₦400million budgeted for EPR in the 2021 and 2022 budgets respectively, will be released.

According to Honourable Magaji Zarewa, the Vice Chairman of the State Assembly’s Committee on Health, the health security bill is one of the priority bills before the lawmakers. “The bill is in its final phase, and will be passed soon,” he said.
Incorporating the One Health Approach
To improve health security, it is critical to adopt the One Health Approach, which addresses the collaborative effort to attain optimal human, animal and environmental health. This was another gap identified by the JEE said Dr. Kauran-Mata. As a result, the epidemic preparedness and response mechanisms in the state have been modified to include stakeholders from both sectors. “We have created an additional pillar on zoonosis in the epidemic preparedness and response policy, headed by a veterinarian from the Ministry of Agriculture. We also have a water, sanitation and hygiene component, which is headed by the Ministry of Environment,” Dr. Kauran-Mata said. He added that during a recent Lassa fever outbreak in the state, both ministries were involved in the response, which helped contain the outbreak.

A state-wide disease surveillance system
Infection prevention and control (IPC) cannot be effective without a comprehensive, bottom-top surveillance system. For Kano State, it involves everyone, from community members and leaders to primary health care centres, all the way up to the state level. “We have community informants who work as volunteers and are linked to health facilities in the communities. Once a disease with outbreak potential is recorded, or rising cases of a disease are noticed in a community, they make a call to the local Disease Surveillance and Notification Officer (DSNO), who immediately goes to the community for further investigation,” said Dr. Imam Wada Bello, Director of Public Health and Disease Control at the State Primary Health Care Management Board.
According to Dr. Bello, periodic training on event-based surveillance is provided for the community informants and local DSNOs, so that they have the skill to detect cases quickly. Each health facility in the state has a surveillance focal person who monitors infectious disease cases and inputs them into the Surveillance Outbreak Response Management and Analysis (SORMAS) system, while also reporting cases of potential outbreak to the DSNO. Plans are also underway to incorporate private health facilities in the state-wide surveillance system. “Once there is a suspected case of any disease with outbreak potential, we make sure that investigations are carried out, and a report prepared within 24 hours so that response can be mounted,” said Dr. Kauran-Mata.
Work to do
Kano State appears to be making progress towards strengthening its health security. This should set a good example for other subnational entities to follow. However, a 46% score in the JEE is still below average, though gaps identified are already being addressed.
As the state works to strengthen epidemic preparedness and response, Kano State lawmakers should prioritise the passing and signing into law of the health security bill, so that processes for its implementation could be set in motion.
Although the State Ministries of Agriculture and Environment are now part of the response to infectious disease outbreaks, authorities at the local government level should be fully involved in the process as most risk factors for infectious disease outbreaks — slaughterhouses, waste management, open drainages, and markets — fall under the purview of local government authorities and are potential ‘ground zeros’ for infectious diseases, if not properly regulated.
This narrative was done as part of the #COVID19NigeriaStories documentation project on state-level responses to COVID-19, implemented by the Nigeria Centre for Disease Control and Nigeria Health Watch with support from the Ford Foundation.
Leave a Comment
Your email address will not be published. Required fields are marked *

