Every millennium has had unique challenges, and some challenges have carried on from one millennia to another. One of such challenges is maternal mortality. For centuries, death has been feared as one of the possible dangers to a woman while giving birth. Although the annual maternal mortality rate has reduced by about 43% from 1990 to 2015 worldwide, this has hardly reflected on the maternal mortality rates in Nigeria. Everyday in 2015, approximately 830 women died from preventable causes related to pregnancy and childbirth. 19% of maternal deaths worldwide in 2015 were in Nigeria.
Maternal mortality is caused by many factors; from eclampsia to prolonged labour to infections. However, Post-Partum Haemorrhage (PPH), defined as loss of more than 500ml of blood from the vagina immediately after labour or within 24 hours after delivery, is arguably the leading cause of maternal mortality in developing countries. Post-partum haemorrhage is caused by excessive bleeding as a result of the uterus being unable to contract efficiently, from vaginal or cervical tears. According to the World Health Organisation (WHO), PPH accounts for one quarter of all maternal deaths worldwide. Providing solutions to PPH, could lead to a reduction of about 30% in maternal deaths, quite a significant figure.

Image credit: Nigeria Health Watch

Post-partum haemorrhage is both preventable and treatable. In its 2012 Guideline for the Prevention and Treatment of Post-Partum Haemorrhage, WHO recommended that all women giving birth should be given “uterotonics” which are medicines used to induce or increase the contraction of the uterus during delivery. Uterotonics include oxytocin, misoprostol and ergometrine. However, because of its proven efficacy and safety, it is recommended that oxytocin be given as the first line drug against post-partum haemorrhage. Oxytocin needs a stable cold chain from point of manufacture to point of use.
These medications which easily prevent PPH are readily available and fairly affordable. Still, the frequency and fatality of post-partum haemorrhage in Nigeria is quite high. To investigate why deaths from PPH remain high in Nigeria, the US Pharmacopeial Convention (USP) in collaboration with the National Agency for Food and Drug Administration and Control (NAFDAC) carried out a survey in 2016 to determine the quality of oxytocin and related PPH drugs in various hospitals and clinics across the six geo-political zones of Nigeria. The survey found that about 74.2% of oxytocin samples in the country failed lab quality evaluations, and 33.7% of misoprostol tablets were found to be of sub-standard quality. This means that 3 out 4 oxytocin ampoules in Nigerian hospitals are of sub-standard quality. In other words, the likelihood that only about a quarter of oxytocin doses administered in Nigeria will have met the required quality standards. Alongside other prevailing factors, this could help explain why Nigeria still has an unreasonably high rate of maternal deaths due to complications from pregnancy and childbirth.
Reducing the circulation and use of sub-standard uterotonics, especially oxytocin injections, may contribute significantly to the reduction of maternal deaths in Nigeria. But before that step, we must first understand why there is such a high failure rate of such an otherwise potent drug in Nigeria, and few questions needed to be addressed. Are oxytocin injections not manufactured properly by the pharmaceutical companies? Is the active ingredient added to the drug not the right amount? Are there problems with the importation and transport systems? Are there issues with the storage systems for oxytocin? Are oxytocin injections administered at the recommended dose by healthcare providers?

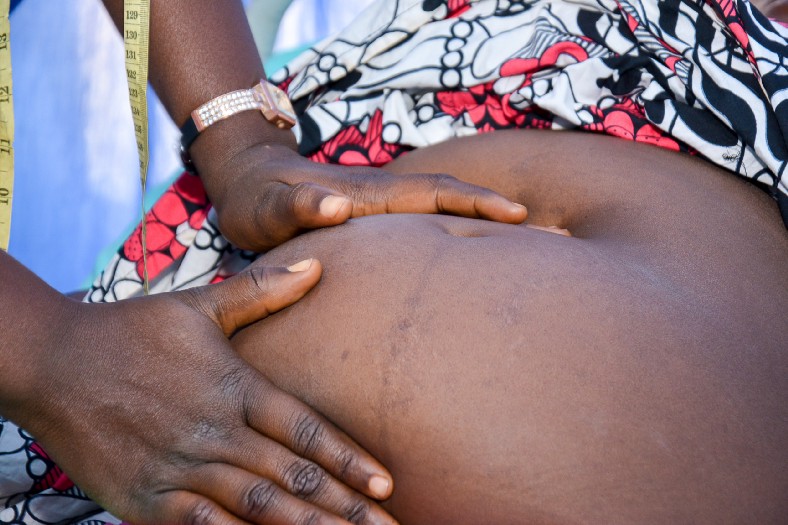
Image credit: Nigeria Health Watch

In a follow up to the survey, the United States Agency for International Development (USAID) – funded “Promoting the Quality of Medicine (PQM)” project, implemented by the U.S Pharmacopeial (USP) Convention, commissioned a team of researchers, led by Dr. Chioma Ejekam of the Department of Community Health, Lagos University Teaching Hospital (LUTH) to examine clinical experiences with regards to the use of oxytocin injections by healthcare providers in Lagos State.
The results of this research were presented in Lagos at a roundtable discussion with the theme “Dissemination of the Clinical Experiences of Oxytocin Quality used by Healthcare Providers in Lagos State” on 20th February, 2018 . The commissioned research revealed the following:
- 41% of healthcare providers in Lagos State have used an oxytocin dose that was higher than the World Health Organisation (WHO) recommendation
- just over 64% admitted that they had no way of reporting the perceived ineffectiveness of the drug
- about 13% of the 705 healthcare providers from public and private health facilities who were interviewed, have at one time or another come across an ineffective brand of oxytocin
The most striking of the findings however, was that only 52% of the respondents knew the proper storage procedures for oxytocin, which is supposed to be stored between 2 –8°Celcius. Dr. Ejekam pointed out during an interview with Nigeria Health Watch that, “If these skilled health workers do not know the proper storage of oxytocin, imagine what the knowledge of the lower cadre health workers would be.”


Prof. Frank Giwa-Osagie at the Dissemination of “Clinical Experiences of Oxytocin Quality used by Healthcare Providers in Lagos State” research in Lagos. Photo credit: Nigeria Health Watch
Renowned Professor of Obstetrics and Gynaecology, Prof. Frank Giwa-Osagie, stressed the need for regulatory agencies to increase their post-marketing surveillance of medications across the country and the enforcement of standard regulatory procedures for the storage of medications in hospitals and pharmacies. The fact that 52% of healthcare workers interviewed did not know the proper storage conditions for oxytocin and 41% have administered oxytocin at a dose higher than WHO recommended guidelines is a serious cause for concern.
While efforts are made to improve the overall supply chain system, storage procedures and administration of oxytocin injections, it could be helpful to also pay more attention to misoprostol, an alternative drug recommended by the WHO and International Federation of Gynecology and Obstetrics (FIGO) for the management of PPH. Because misoprostol is administered orally, it does not require administration by a skilled healthcare professional, and it can be stored at room temperature without losing its efficacy. These factors mean that misoprostol has less of a failure rate than oxytocin in Nigeria. As Prof Akinola, current President of the Society of Gynaecology & Obstetrics of Nigeria (SOGON) mentioned during the Lagos USP meeting, there are a number of potential product options for the prevention and treatment of PPH, however they’re only useful if they’re good quality products.
Dr. Chimezie Anyakora of U.S Pharmacopeia Convention, mentioned that they plan to expand the Clinical Experience of the use of Oxytocin Survey to cover more states across the length and breadth of Nigeria, to unearth more significant findings that will help in reducing post-partum haemorrhage when oxytocin is administered in Nigeria.
It could also be useful for the US Pharmacopeia Convention to include other uterotonics such as ergometrine and misoprostol in the Nationwide Clinical Experience Survey they intend to conduct on oxytocin. By understanding the experience of different healthcare providers from all regions of the Federation, we will have a more flexible and robust approach towards the use of specific medications for the prevention and management of PPH.
These findings, though only from Lagos State, reveal the task ahead for Nigeria if it is to reduce maternal mortality through the proper use of oxytocin. All participants at the dissemination discussion agreed that there is an urgent need to revolutionize the Drug Supply Chain System in Nigeria. From challenges of standard procurement practices, to the arrival of the medications at the ports, to the vehicles conveying them to different locations across the country, to the pharmacies and hospitals where these drugs are stored before use, care must be taken to ensure that the right storage conditions are maintained for this vital drug to ultimately save Nigerian women from dying from complications after childbirth.


It’s more shocking because medics are usually confused when after administering oxytocin the required results aren’t achieved.
This is a fantastic write up. It’s an eye opener. It’s a must read for all practising medics in Nigeria.
This document should be circulated as wide as possible for the eventual benefit of all doctors and patients.
This is painful to read.
Why is this still a big deal in Nigeria?
Do our leaders not know these things or have they not lost anyone even remotely known to them that would encourage them to invest in this very natural business called child birth?
I was writing a paper for my school yesterday and then I stated that Nigerian pharmaceutical companies are the ones killing the health sector of the country. I talked about insecticides and malaria medicines that are not effective and yet these companies keep making a fortune by selling fake drugs. Here is another one. What can we do now??
With the poor power availability, there is a serious challenge of oxytocin storage especially in rural hospitals where majority of the women deliver.
In order to reduce the incidence of serious obstetric haemorrhage and mortality, misoprostol should replace oxytocin as the first line drug. Is this in practice?
So glad with the write up