A blue Toyota Corolla pulled to a stop inside the hospital premises and a middle-aged woman helped a frail young boy into the outpatient unit. She approached the nursing station with a distressed look on her face. A member of staff from the hospital took the boy into the nursing station to attend to him.
“What happened to this young man? Cold de catch you? Who carry am come? Wetin de do you?,” a young doctor asked as he walked briskly towards the nursing station. He sanitised his hands, wore his stethoscope and listened to the boy’s heartbeat. “Can we get a wheelchair?”, he demanded. An elderly man appeared almost immediately with it and wheeled the boy into the ward.
A frantic effort to save his life started as he began gasping for air. He was given oxygen. The laboratory staff struggled to collect his blood sample as it was difficult for them to find a vein.
They eventually succeeded in collecting a blood sample, and it turned out the boy was anaemic as he had a low red blood count and required a blood transfusion. A hospital visitor volunteered and the boy was able to be transfused. Some colour returned to his pale features and his mom managed to smile again, thanking the voluntary blood donor with a malt drink.
Quality care in an unexpected place
You would imagine the emergency described above happened in a fancy health facility in a city. But it happened in the unlikeliest of places, a general hospital in Kolo, a rural community 20-minutes from Oloibiri in Ogbia Local Government Area (LGA) of Bayelsa State, about 28km southeast of the state capital and a major health care hub for communities around Yenagoa.

The first discovery of oil in commercial quantities in West Africa was in Oloibiri in 1956. A number of controversies still surround the area and indigenes complain that they have nothing to show for the vast natural resources that lie beneath their feet that has contributed to the growth of nation.
Even though Primary Health Care (PHC) is regarded as the bedrock for achieving Universal Health Coverage (UHC), there has not been commensurate investment to it. With support from partners, Nigeria launched the Primary Health Care Under One Roof (PHCUOR) initiative in 2011, a reformation policy to integrate and improve service delivery at sub-national levels. Bayelsa performed abysmally in a 2012 scorecard that assessed the implementation of PHCUOR across different dimensions of the policy. The state scored five percent, the fifth out of six south-south states while neighbouring Rivers State, another oil-producing state, scored 73%. The hospital that saved the young boy’s life probably wouldn’t have been able to carry out the blood transfusion 12 months ago as it only started operations in late 2018, thanks to the intervention of the Shell Petroleum Development Company of Nigeria (SPDC).
In 2014, Shell, a major stakeholder in the region, developed a plan to address the low health indices and to improve health care delivery for the communities of the Ogbia LGA in Oloibiri field. Named after Oloibiri and used to commemorate Nigeria’s centenary celebration, the Oloibiri Health Programme (OHP) is a well-planned, multi-phase intervention by the company, its partners and the Bayelsa State government, aimed at redefining sustainable primary healthcare in Nigeria.

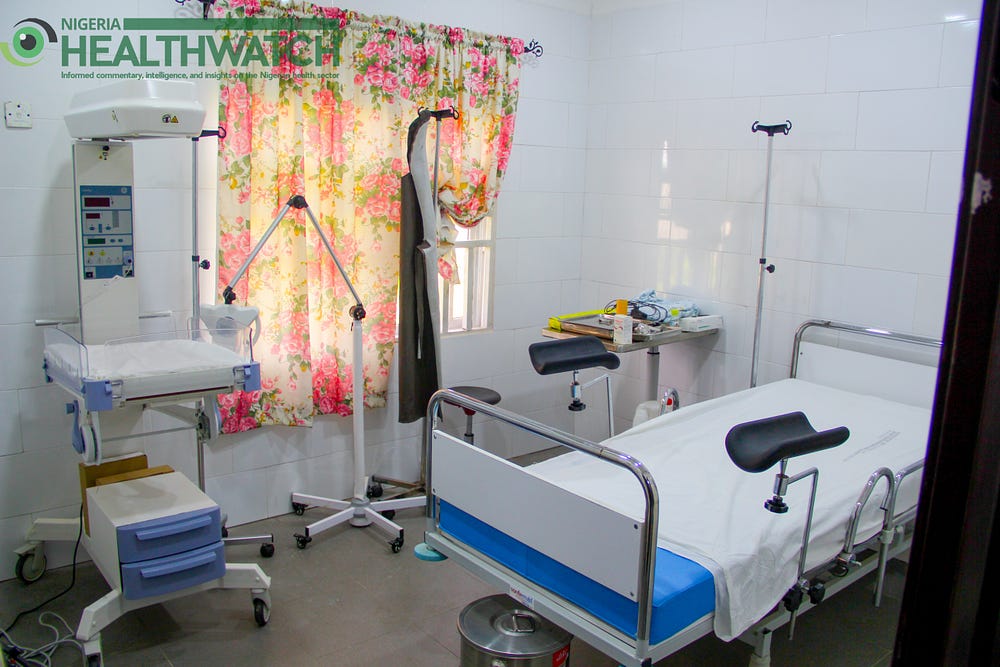
The first phase, which has been completed, includes revamping the previously defunct Kolo General Hospital; construction of a 10,000 litre water treatment plant within the hospital; purchase of medical laboratory equipment for the College of Health Technology Otuogidi; and donation of a dental chair to Demonstration Clinic Otuogidi.
Kolo General has steady access to electricity, with a standby 33KVA generator and a hybrid solar-powered system; a well-equipped and aesthetically pleasing maternity ward and delivery room, male, female and children wards. It runs an electronic health records system; the fully equipped laboratory operates a mini blood bank and the radiology unit has ultrasound and mobile x-ray machines.
This phase is already tackling the problem of accessibility to quality healthcare, availability of a constant water supply, human resources for health and dental health, a major disease of inequality.
A Model that’s built to last
The OHP is a different model of Public-Private Partnership (PPP) as it incorporates an extra “P” — the people. It has an ambitious vision of changing the narrative that most primary healthcare centres cannot provide essential services.

The OHP model could potentially be a reference point for achieving UHC using primary health care delivery as a springboard. Dr. Olumide Okunola, who works with the International Finance Corporation (IFC) of the World Bank, one of the project’s partners, described Ogbia as “the first community to achieve universal health coverage in Nigeria,” because the OHP adopts a holistic approach that doesn’t focus only on constructing buildings, but provides water, power and other critical elements needed for optimal performance.
Bayelsa State Deputy Governor, Rear Admiral Gboribiogha John-Jonah Rtd., recognised sustainability as a major problem of several big projects when he said “It’s one thing to start, it’s another to sustain. Sustainability is key and it’s our hope that the project will be sustained over the years to alleviate the health challenges of all Bayelsans”.
Shell already started thinking about sustainability from the beginning and plans to run the hospital in a “financially sustainable way”, explained Dr Akinwumi Fajola, Shell’s Regional Community Health Manager.
He said the OHP is expected to increase healthcare coverage for underserved communities, reduce the number of mothers dying in childbirth, reduce the number of children dying before the age of five, reduce the prevalence of water and sanitation related illnesses, and improve the quality of life and life expectancy of individuals within the communities.

The beauty of the OHP, said Dr Fajola, is how it complements existing state, national and international health programmes, especially the Saving One Million Lives (SOML) initiative of the Federal government. Other phases of the OHP include a medical store to support the operation of a sustainable drug revolving fund, a health campus in Oloibiri town, a knowledge management centre, an access road to the health facilities and a Foundation to sustain the programme.
Shell is not new to ensuring equitable access to healthcare having successfully implemented a similar project at Obio Cottage Hospital, Rivers State. The final phase of the OHP involves establishing the Ogbia Health Insurance Scheme, which will be modelled after the pilot at Obio.
Improving Cancer Care in Nigeria
If the Oloibiri Health Programme is a demonstration of Shell Nigeria’s interest in improving the health of Nigerians, its multi-billion-dollar Linear Accelerator (LIAC) Radiotherapy machine recently launched at the National Hospital Abuja is a confirmation of this commitment.
There are many stories of both financial and mental woes of Nigerian patients diagnosed with various forms of cancer. The lack of radiotherapy machines for treatment in Nigeria has led to as many as 70, 327 deaths. Even though the government is responding within its capacity, cancer continues to be a leading cause of death across the globe, leading to 15% (7.6 million) of all deaths in 2008 with 66% in low-and middle-income countries like Nigeria. The projection is grim, with 13.1 million deaths from cancer estimated by 2030 if the rise continues.

The people who make up these statistics are like Chidi’s (name changed to protect privacy) mum, who lost a long battle with cancer in 2016. Life has never been the same in their two-bedroom apartment in Enugu State. Another is Mr Frank who left behind his new wife and son after a debilitating fight with stomach cancer. Prevention and early detection of cancer have always been the focus of advocacy by both government and non-governmental organisations. But when these fail, fast and effective treatment is the best thing a patient can hope for.
The Shell Nigeria Exploration Company of Nigeria (SNEPCo) in partnership with the Nigerian National Petroleum Corporation (NNPC) recently donated the radiotherapy machine to the hospital. The Hospital’s Chief Medical Director, Dr Jaf Momoh, said the second machine will transform cancer treatment in the hospital as patient treatment will no longer be interrupted during routine equipment maintenance.
Beyond providing the infrastructure to improve patient care, the partnership built the capacity of health workers to operate and maintain the machine, Mr Bayo Ojulari, the MD of SNEPCo, said. This helped build a skilled health workforce critical to the operation and maintenance of the radiotherapy machine. A leading medical equipment company in Nigeria, JNC International, provided technical support during its installation as the official representative of the manufacturer, Elektra.
Mr Ojulari said the machine employs a unique treatment technique that specifically targets and destroys cancerous cells with minimal adverse effect on surrounding organs. There is often a need to weigh up the benefits and risks of radiation therapy as well as to take into careful consideration the safe level of radiation therapy that is necessary for each individual patient.
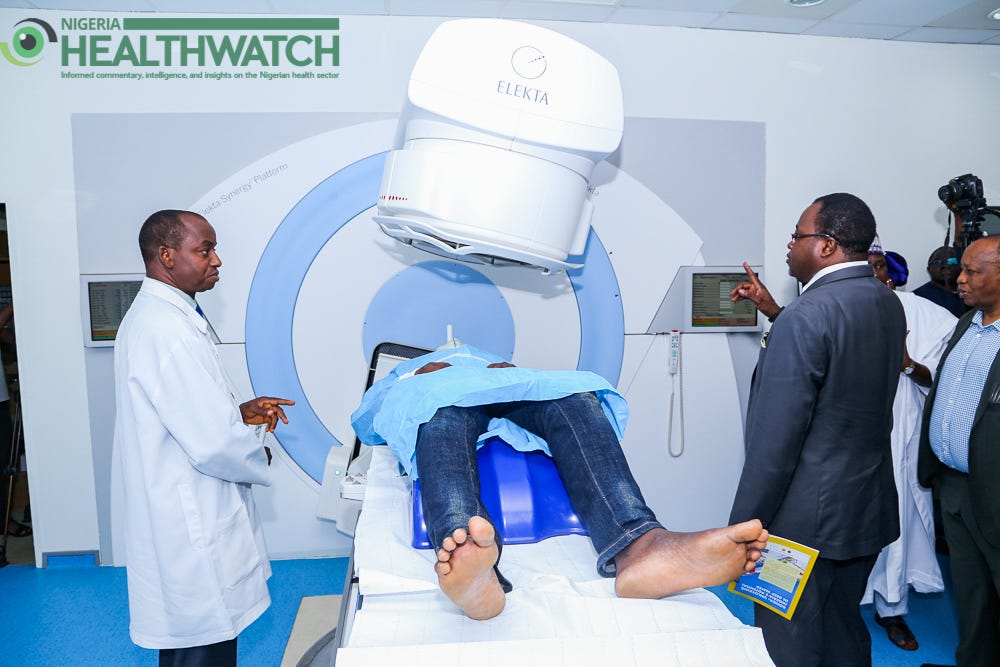
Dr Momoh said the treatment is also more affordable, at a cost of $2000 compared to Ghana where costs are as high as $10,000 for the whole treatment regimen. He also said the waiting time for treatment will be significantly reduced. Time is an important factor in cancer treatment as unlike most illnesses, cancer cells are not stationary but can spread to other parts of the body quite rapidly, reducing the patient’s chances of survival.
The need for cancer care financing in Nigeria
Implementing Nigeria’s National Cancer Control Plan (2018–2022) is estimated to cost 97 billion Naira, with the government providing 75% of the funds and the rest to come from donors and development partners.
The private sector is already showing enthusiasm, but government must lay a proper foundation. An alternative model for financing a cancer treatment facility, is the Nigerian Sovereign Investment Authority (NSIA) and Lagos University Teaching Hospital (LUTH) Cancer treatment centre. This is PPP between the NSIA and LUTH will see full ownership of the cancer facility revert back to LUTH after a 10-year period.
If you consider Nigeria’s population and the estimated rise in cancer cases, in the next decade, there will be a significant shortfall in the number of available radiotherapy machines to manage the growing cases of cancer. The cost of $2000 for treatment at the National Hospital Abuja is still out of reach for a significant number of Nigerians, so while treatment is available, it is not necessarily accessible, especially for the poorest of Nigerians.
This cost factor is one reason the Catastrophic Health Fund (CHF) was conceptualised, the WB/IFC’s Dr Okunola said. “Within the context of Universal Health Coverage, the role of public financing is sine qua non to make healthcare available for all, then we must prioritize access for the poorest of the poor. In this regard there has been progress on this front as the Basic Health Care Provision Fund (BHCPF) makes more public financing available for basic health services,” he said.
He noted that there needs to be similar progress in terms of non-communicable diseases (NCDs), and the CHF was proposed to ensure that just as basic health services were being publicly financed, NCDs such as cancer should also have a public financing mechanism. “The idea behind the CHF is to; allow the poor and vulnerable to access very expensive cancer care; allow the private sector make the necessary investments because they are sure of payment; and when more cases are treated, then human resources for health will be able to get more skills and capacity building in country, and the more they do, the more the prices will come down,” he said. The CHF was pushed by former Chair, Senate Committee on Health, Senator Lanre Tejuoso, and Okunola noted that current Chair, Senator Ibrahim Yahaya Oloriegbe, has said the CHF is one of his priorities.
There is a popular saying that “little drops of water make a mighty ocean.” Shell’s “people-centred” health investments are important steps that highlight the critical role the private sector can play in supporting the health sector. Alongside efforts from other stakeholders, this should put Nigeria on course to achieve universal access to quality and affordable healthcare for all its people, not only from Oloibiri to Abuja… but from Abia to Zamfara.
Do you know of other innovative private sector investments in primary, seondary or tertiary care? Let us know in the comments or on the Nigeria Health Watch social media platforms.



I am impressed about this information and will like to be added in the mail update on health information.