By Josephine Chinele (Lead Writer)
Her priest’s announcement was enough reason for Cecelia Yohane, a resident of Nchalo Chikwawa, to have her 2-year-old grandchild vaccinated against polio. “All my children are not educated, not many people in my village are educated either. But I want to change our story through my grandchildren. I want this particular one to become a teacher hence my interest to have her protected from any life-threatening diseases,” she said.
30 years after the last case of wild poliovirus, the Malawian government announced its re-emergence in February 2022. This was the first case in Africa since the region was certified free of indigenous wild poliovirus in August 2020. The confirmed case of wild poliovirus was a 3-year-old girl in the country’s capital, Lilongwe, who became paralysed as a result of the infection.
Yohane was devastated by this news as it threatened her plans for her granddaughter. She decided to go ahead and vaccinate her granddaughter against the disease, even though she had already received the same vaccines through her routine immunisations.
“Our priest encouraged all congregants with children under five years to have them vaccinated against the deadly disease. This was my first time to hear him talk about a mass vaccination campaign, enough confirmation that this is a deadly and distressing disease,” Yohane recalled.

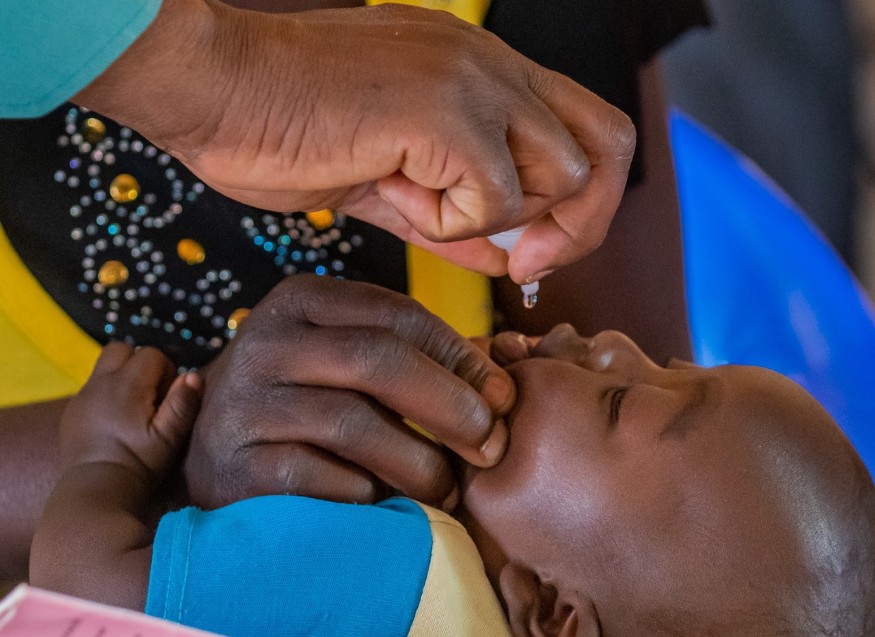
Poliomyelitis is a viral disease which invades the nervous system and can cause total paralysis within hours, particularly among children under 5 years. While there is no cure for the disease, it can be prevented through the administration of a safe, simple and effective vaccine.
For decades, African governments fought to eradicate the virus and in August 2020, the continent was certified free of indigenous wild poliovirus. The Malawian case is the first on the continent since then. The World Health Organization (WHO) says “the region’s certification as wild poliovirus-free remains unchanged” because “laboratory analysis linked the strain detected in Malawi to the one circulating in Pakistan’s Sindh Province”.

In March 2022, Malawi launched the first round of door to door mass polio vaccination campaign targeting 2.9 million under five children. According to the WHO, more than 80 million doses will be administered to more than 23 million children under 5 years in the four-round vaccination drive in five southern African countries, after Malawi reported the case. A WHO statement stated that the first phase of the campaign targeted 9.4 million children in Malawi, Mozambique, Tanzania and Zambia, “Three subsequent rounds — in which Zimbabwe will also take part — are set for April, June and July.”
Swift intervention
Ministry of Health (MoH) Spokesperson, Adrian Chikumbe said, even though the country achieved eradication, the ministry continued with surveillance as neighbouring countries still registered some cases. Through routine surveillance, a suspected case was identified in Lilongwe. Since Malawi doesn’t have laboratories for this type of investigation, a specimen was sent to South Africa for testing. The results came out positive.
The MoH activated mass vaccination campaigns, ensuring that all children received the required dose of bivalent oral polio vaccine (bOPV). Chikumbe acknowledged that the campaigns have been successful due to collaboration between the ministry and various other stakeholders, “most importantly, religious leaders, considering that there is a history of children missing out on vaccinations due to their religious beliefs.”
He added that surveillance on acute placid symptoms of wild poliovirus was still ongoing alongside the vaccination campaign. Specimens were sent to South Africa, but all tested negative. “We have two more polio mass vaccination campaigns in May and June. After we complete the mass vaccination campaigns, we will continue with the routine vaccination campaign at under-five clinics. Even during this campaign, we have continued to provide routine immunisation,” he said.

The mass vaccination campaigns are courtesy of the MoH and its partners — Global Alliance for Vaccines and Immunisation (GAVI) and the United Nations International Emergency Children’s Fund (UNICEF).
Foot soldiers
The two rounds of door to door vaccination campaigns have been made possible through the dedicated efforts of Community Health Workers (HSAs). Carrying the polio vaccines in portable coolers, the HSAs go from door to door in every community, to ensure that they reach all eligible children.
The HSAs brave all kinds of weather to achieve maximum coverage. Chikwawa (located in southern Malawi) is a generally hot district and they sometimes walk five kilometers a day, moving from village to village. When they run out of supplies, they have to walk back to the nearest facility to collect more vaccines. HSAs are paid MK6, 000 ($7.4) as lunch allowance every day but they usually receive this months later when funding becomes available. Despite these challenges, they display a remarkable dedication to their work.

“The first round was the toughest as rivers were still flooded following Cyclone Ana and Gombe. In the second round, it was better but very hot” said Sydney Labeka the Senior HSA for Chikwawa Nchalo area.
“In both rounds, we missed Chikuse Island which is on Shire River (Malawi’s biggest river) because it had high water levels. There are certain places we used to cross the river but after the floods, these areas have a lot of crocodiles. The area’s traditional leaders advised that we should wait,” he added.
Chikwawa District Hospital spokesperson, Settie Piriminta said the second vaccination campaign round achieved 82 percent coverage. This was somewhat lower than the initial campaign and he attributed it to some system challenges like “insufficient fuel for supervision and our HSAs complained of walking long distances to administer the vaccines”.
Collaborative effort
According to UNICEF Malawi Child Health Specialist, Lokesh Sharma, UNICEF is impressed with the campaign as, in both the rounds, Malawi was able to achieve the desired vaccination coverage.
As partners, UNICEF has provided technical support, creating an emergency operation centre at the Expanded Programme on Immunisation (EPI) within the MoH to coordinate the Wild Poliovirus Outbreak Response (WPV1 OBR). They also provided 6.9 million doses of bOPV and ensured that all levels of the cold chain had capacity to keep vaccines in the proper temperature range and to maintain their efficacy.
“In response to the bOPV campaign, UNICEF made sure there were no myths or misconceptions in the community. We assisted in the planning and development of the many pieces of communication. These include radio jingles, press release statements and more. UNICEF also helped with district official training,” said Sharma.

Father John Chitsul, Parish Priest at Saint Pius Catholic Church in Blantyre, makes it a practice to call on fellow religious leaders to take an interest in health issues and jump on campaigns such as this. “God doesn’t want a person to suffer but to live a healthy and peaceful life. Hence my encouragement to parents to have their children vaccinated against the disease. We need to work together to fight these pandemics,” he said.
Non-stop effort
Head of Community and Environmental Health at Kamuzu University of Health Sciences, Blantyre, Malawi, Professor Adamson Muula said the Ministry of Health has done well in mobilising and ensuring that under five children receive bOPV, “Many districts have exceeded their targets while some, especially Chikwawa have not. Programmatically there have been challenges but the MoH and its partners are continuously addressing these challenges. At the end of the day, it appears to me that the country will be proud of its campaign.”
In April 2022, the Global Polio Eradication Initiative (GPEI) launched the 2022–2026 strategy: ‘Delivering on a Promise‘, which aims to vaccinate 370 million children annually for the next five years. It promises to ensure continued global surveillance activities for polio and other diseases in 50 countries.

Thanks to the MoH’s swift action, Malawi is once more polio free. But because the world is in constant danger of emerging and reemerging infectious disease outbreaks, there is a need for continuous surveillance and innovations to ensure that eradicated diseases like polio remain eradicated. The implementation of GPEI’s strategy is an ideal way of preventing such future outbreaks.