It was the last day of 2019. Everyone, including health workers at Aminu Kano Teaching Hospital (AKTH), the largest healthcare facility in Kano State, looked forward to the New Year.
Salamatu, a 28-year-old woman, 38 weeks pregnant, arrived at the Obstetrics & Gynaecology (O&G) unit on referral from Standard Hospital, a private hospital where she attended for her antenatal classes. She had been in labour in the private hospital and sensing she could be having some complications, the health workers referred her to AKTH. Besides feeling weak, she had a fever with mild bleeding. Upon examination, the medical team decided to carry out an emergency Caesarean Section (CS). A team of six including Consultant Anaesthesiologist, Dr. Habib Muhammad and House Officer Dr. Ummulkulthum Abba operated on Salamatu. Unfortunately, the baby had died before the surgery and Salamatu herself suffered a cardiac arrest immediately after the surgery. She was resuscitated and transferred to the Intensive Care Unit (ICU) where, sadly, she died on New Year’s Day.
The events that followed confirmed Salamatu to be Kano State’s index case in the current Lassa Fever outbreak in Nigeria. She had traveled to Bauchi State two weeks before to take care of her ill mother, who later died. Upon returning to Kano a few days later, she fell ill and was taken to Standard Hospital, where she went into labour. What was thought to be at first a case of malaria, turned out to be Lassa fever, the deadly viral haemorrhagic fever infection that has so far in 2020 resulted in 472 confirmed cases with 70 deaths in 26 states across the country, according to the latest data from the Nigeria Centre for Disease Control (NCDC).

Fear, anxiety and a series of unexplained deaths
Seventeen days after Salamatu’s demise, Dr. Abba, who had just finished her medical degree and was undergoing the mandatory one-year internship program, fell ill and had a fever. She was admitted at the retainership ward of AKTH but died within hours. Three days later, Dr Muhammad also fell ill with the same symptoms. He later died. ‘’This created serious panic in the hospital,’’ says Prof. Abdurrahman Sheshe, the Chief Medical Director (CMD) of AKTH. ‘’Fear gripped everyone. Patients on admission were requesting to be discharged and people stopped coming to the hospital.’’
Almost immediately, the possibility of a serious viral infection, most probably Lassa fever, was suspected. The hospital alerted the state Public Health Emergency Operations Centre (PHEOC). Dr. Muhammad’s blood samples, which were collected and sent to the hospital laboratory before his death, were retrieved and sent to the NCDC reference laboratory in Abuja to be tested. Three days after, it was confirmed that he died of Lassa Fever.

The race against time
‘’It was like a time bomb. We had to trace every person that had contact with the deceased,’’ Dr. Bashir Lawan, the State Epidemiologist and head of the PHEOC, said. The contacts were grouped into three categories:
- People who had direct body and body fluid contact with the cases without any protection, the third category.
- People who had direct body contact with the cases while wearing protection, the second category
- People who had minor or indirect contact with the cases, the first category.
Disease Surveillance and Notification Officers (DSNOs) and other PHEOC staff traced a total of 318 contacts. The NCDC also sent a team to provide technical support. The third category contacts received Ribavirin, a preventive antiviral medication for the infection. The NCDC sent medications and some Personal Protective Equipment (PPEs) and distributed them to hospitals across the state, including AKTH. The medical team closely monitored identified contacts, checking their temperatures twice a day. Contacts in the first and second categories were each provided with thermometers to self-check their temperatures twice a day as well. They received training on Lassa Fever symptoms and techniques of checking their temperatures using the thermometers and were given numbers to call if they start experiencing symptoms. Contacts who could not read or write were assigned personnel to assist them. Phone numbers of all the contacts were collected for periodic check-ins.

As this happened, the state ministry of health and the management of AKTH made plans to manage the fear of Lassa fever. ‘’We conducted a series of sensitisation and training sessions on infection prevention and control for all staff of the hospital. We also put in place hand washing facilities at strategic places in the hospital,’’ says Rabiu Alhassan, head of the Infection Control Unit of AKTH, adding that, ‘’Tension was really high among staff and we had to douse it.’’ The state produced and aired radio jingles on major stations. Community sensitisation visits were initiated in all wards across the state to douse fear and raise awareness about the disease and how people can protect themselves. Health workers in state-owned hospitals were sensitised on IPC and the need to maintain high index of suspicion. A burial committee was also established to handle safe burials of the deceased.
A small isolation centre for a rather big state
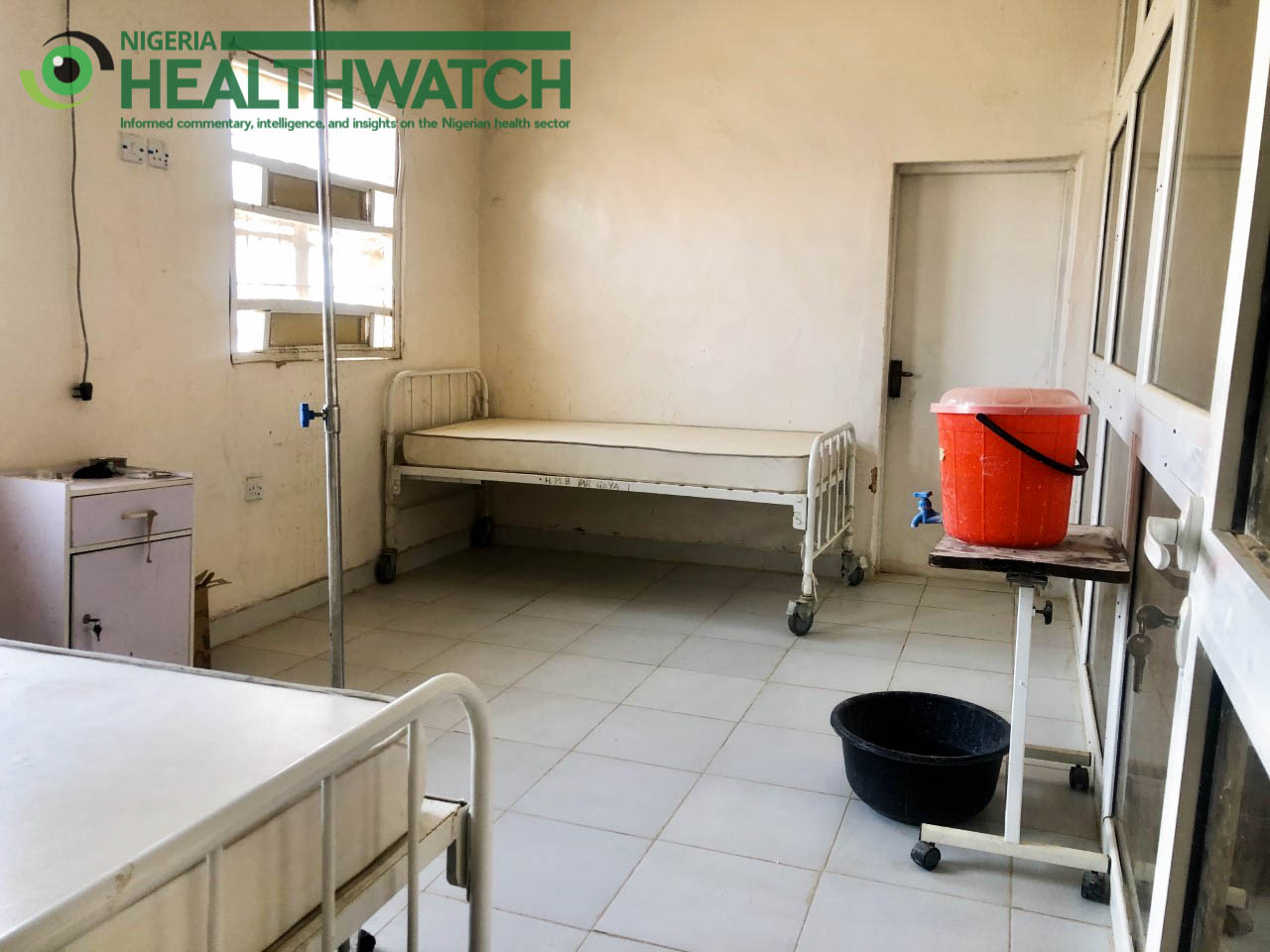
As the state raced to trace and monitor contacts, two more staff of AKTH who were already under monitoring fell ill with similar symptoms to their late colleagues. The two staff, an theater nurse and a doctor, both had contact with the late Salamatu. Despite AKTH being a tertiary healthcare facility, there is no specific isolation centre where cases of highly infectious diseases can be managed. The patients were taken to the state’s isolation centre in Yargaya town along Maiduguri road on the outskirts of Kano city.

Kano state is one of the most populous states in Nigeria with a projected population of over 13 million people. It is one of the country’s commercial centres with thousands of people transiting through the state daily, increasing the potential for infectious disease outbreaks. Yet the state has only one isolation centre to manage suspected and confirmed cases of infectious diseases.
Built in 2014 during the Ebola outbreak in Nigeria, the Yargaya isolation centre is a 14-bed facility managed by six staff. It has three wards, with two serving as isolation wards for highly suspicious and symptomatic cases and one for confirmed cases. The centre has been used in the past to manage outbreaks such as Monkeypox, according to Dr. Abdullahi Anifowose, a medical officer at the centre. Presently, the centre is being used to manage Lassa fever.
The two health workers from AKTH were admitted here while waiting for results of their tests. One of them tested negative and was discharged, and the other who tested positive is receiving treatment alongside another doctor brought in from neighbouring Jigawa state.
Isolation centres play an important role in managing infectious diseases outbreaks, and a densely populated state like Kano with its commercial status needs more than one. What if there is need to isolate more people than the Yargaya centre can accommodate? What if a suspected case is from a faraway local government and will take long to reach Yargaya? It would be more efficient to have one centre in each senatorial zone to reduce the risk of an infected person losing their life as a result of long-distance travel. Kano’s experience should serve as a wakeup call to other states where isolation centres are not available. If the Yargaya isolation centre did not exist, the health worker from Jigawa state may not have had another centre to go to for treatment. All states should have their own fully equipped, well-staffed isolation centres to better manage outbreaks.
Protection in the line of fire
Usually the first to provide care to patients, health workers are always exposed to infections, and protective measures such as PPEs are not always available. A number of health professionals have lost their lives while caring for their patients.
While it is their duty to save lives, it is important that hospitals reinforce to health workers and all their staff the need to protect themselves by practicing Infection Prevention and Control (IPC) procedures. Hospitals and ministries of health must always make available the basic PPEs to staff, and ensure a stringent hygienic environment in and around health care facilities as outlined by the NCDC in its Lassa Fever Healthcare Workers Advisory. Also, hospitals need to carry out periodic training for their staff on IPC and emphasise the need to maintain a high index of suspicion especially while attending to patients with symptoms of deadly infectious diseases.

The ability is there, the infrastructure is missing
“We have the personnel to carry out tests and manage cases of deadly infectious diseases like the Lassa fever, but the needed infrastructure is not there’’, says Dr Sheshe. AKTH neither has the laboratory capacity to test for Lassa Fever nor an isolation ward to manage suspected and confirmed cases. He said a request has been made to the Federal Ministry of Health to construct a laboratory in the hospital that could serve as a reference test centre for the north-west region. He adds that a budget proposal will be submitted to the ministry for the establishment of an isolation centre in the hospital. The Federal Government has a duty to ensure that budgets are appropriated and released to build the capacities of our national public health institutions and health care facilities to effectively prevent and manage infectious diseases outbreaks early.
Governments must be deliberate to fight infectious disease outbreaks
Kano state has lost three persons to the current Lassa Fever outbreak, including two health care professionals working hard to provide care to their patients. The state made a wise investment in 2014 by building the Yargaya isolation centre, which is now helping to contain Lassa Fever. In the course of preventing outbreaks, it is always best to plan ahead, invest in critical areas of prevention and build capacities to respond effectively.
The presence of a PHEOC in Kano State, set up with support from NCDC, has played a critical role in coordinating response to the current outbreak. Kano and other states must however begin to make deliberate investments by appropriating and releasing funds for infectious diseases outbreaks and response. If AKTH and Kano State were prepared for epidemics, they should not have waited to receive Ribavarin from the NCDC. Lassa Fever is endemic in Nigeria and Ribavarin, the drug of choice for its treatment should be available in all hospitals across the country. Budgeting and releasing funds for epidemic preparedness will better allow for capacity building of personnel for continuous surveillance and response, and availability of critical infrastructure to identify and manage cases before they spread.
Do you know what your state is doing to prepare for infectious disease outbreaks? Does your state have an isolation centre to manage cases of infectious diseases? Does your state have a budget line for epidemic preparedness? Let us know on our social media platforms!


Of all the stories about Lassa Fever, this Kano story touched me in the very sore spot of my heart, because we lost such young and dedicated people, and because this is not the first time and pardon me, this will not be the last time that we will uncaringly lose our best. Whose heart will not bleed at seeing the pictures of the late Drs. Ummulkulthum Abba and Habib Muhammad? Who will not shed a tear drop or two, knowing that this wastage of life should not have happened? Tell me who will not wonder why Nigeria, 51 years after the first reported case of LF, still “murders” her health workers by not providing the basic essentials needed to prevent such calamities? We have seen such horrendous loss of health workers before- first in 1969-1970 in Jos, then 1974 in Onitsha, then 1989 in Ekpoma, Owerri, Aboh Mbaise, then 2012 in Abakaliki , then on, and on, and on in other unreported episodes and now in 2019-2020 in Kano. One is tempted to ask- for how long and where next? What type of country is this? Which type of government do we have? I have said it before and I will say it again: Until Lassa fever snatches a life of and Aso Rock resident or the National Assembly holds a one minute silence and suspends a session in memory of a honourable member dead of LF, Nigeria will every year continue to lose her best and talented. My condolences to the families of Drs. Ummulkulthum Abba and Habib Muhammad, as well as to all the families that have suffered in the hands of LF. Enough is enough…Let us invade the NASS with the pictures of all who have died of LF in this country these past 51 years. Perhaps this action may touch the cold hearts of our leaders to positive action. Finally, it is not enough to continue building capacity, without creating the right and conducive environment for the built capacity to function maximally and efficiently. The current Nigerian environment is nothing but a toxic and killing field for built capacity…and yet we want those in the diaspora commit suicide by coming home to their death!
Thank you, Prof. Tomori.
It is indeed very sad that we keep losing health workers and other citizens to Lassa fever every year. Governments at all levels must rise up to the responsibility, budget appropriately and release funds to prepare and respond to outbreaks. Hospitals must also be deliberate in sensitizing health workers to maintain high index of suspicion while attending to patients with cardinal symptoms of Lassa fever. The hospitals must also make available the required PPEs for use of health workers