By Folakemi Ajala (Lead Writer)
From the old (smallpox) to the new (COVID-19), for centuries, vaccines have helped save and promote healthier lives for people of all ages. In the last 2 decades, major gains in the development and production of vaccines have helped prevent more than 20 life-threatening diseases.
Africa was declared wild poliovirus-free in 2020. Over 40 African countries have eliminated maternal and neonatal tetanus, and vaccines are making a huge impact on diseases like cervical cancer, hepatitis and Ebola. While this is notable progress, the reality remains that within health systems in Africa, access to affordable and sustainable vaccine access remains a challenge.
African Vaccination Week
African Vaccination Week (AVW) is an annual event that is celebrated during the last week of April in synchronisation with other World Health Organization (WHO) Regions and the World Immunisation Week (WIW). It is an initiative that has proven particularly effective in bridging the vaccine access gap by reaching populations with limited access to regular health services, as well as, providing an opportunity to integrate other interventions with immunisation services.
It is coordinated by the WHO Regional Office for Africa and implemented by countries. Their goal is to strengthen immunisation programmes in the African region by increasing awareness of the importance of every person’s (particularly every child and woman) need and right to be protected from vaccine-preventable diseases.
This year, the West African Institute of Public Health (WAIPH), with the support of the Partnership for Advocacy in Child and Family Health at Scale (PACFaH@Scale/PAS); a Bill & Melinda Gates Foundation health and social accountability reinvestment project, in collaboration with other partners, hosted a high-level symposium to mark this year’s AVW. The theme was ‘Equitable Vaccine Access, Resilient Communities’.

Equitable vaccine access
According to the Centres for Disease Control and Prevention (CDC), health equity is achieved when every person has the opportunity to “attain his or her full health potential” and no one is “disadvantaged from achieving this potential because of social position or other socially determined circumstances.” Ensuring equitable vaccine access is an important part of achieving the human right to health.
The COVID-19 pandemic served as a reminder to the world that vaccines are critical tools in the fight against diseases, however, studies have shown that even though immunisation positively impacts health (SDG3) and contributes to 14 out of the 17 Sustainable Development Goals (SDGs), such as ending poverty, reducing hunger, and reducing inequalities; sub-Saharan Africa still lags behind.
Therefore the endorsement of a new global vision and strategy by the World Health Assembly, called the Immunisation Agenda 2030 (IA2030) is crucial and timely. IA2030 envisions a world where everyone, everywhere, of every age, fully benefits from vaccines to improve health and well-being. It aims to maintain hard-won gains in immunisation, recover from the disruptions caused by COVID-19, and achieve even more — by leaving no one behind, in any situation or at any stage of life.
During his presentation, Professor Oyewale Tomori, past President of the Nigerian Academy of Science and Former Vice-Chancellor at Redeemer’s University stated that the reason people are left behind is inequity. To level the playing field, he recommended that Nigeria and other African countries need to bring value to the global table in terms of vaccine production. This involves strengthening the vaccine learning ecosystem, and governments taking responsibility for their failures in governance, and committing to correcting them. “If our resources are properly managed, no one will be left behind. More epidemics are coming; we need to be prepared,” he added.

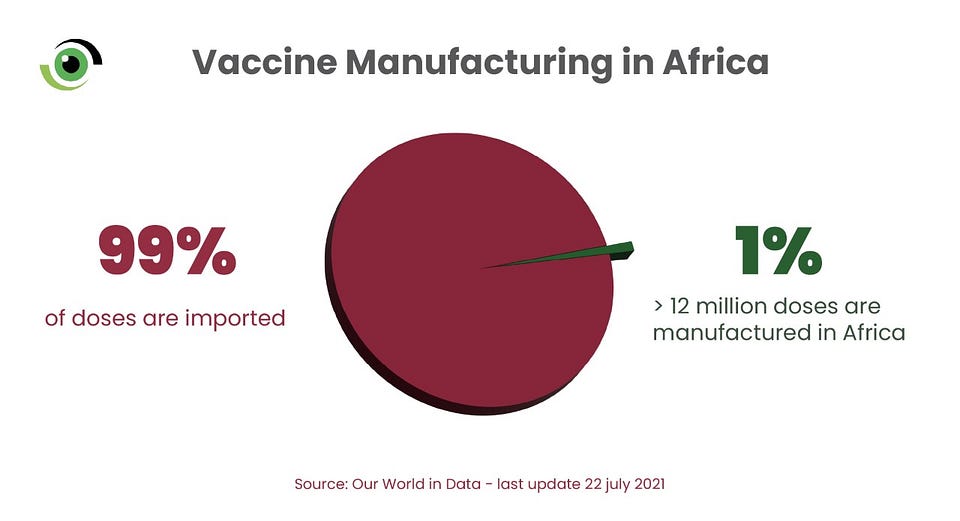
Africa relies heavily on vaccine imports as 99% of the vaccines used within the continent are imported. But this wasn’t always the case. Professor Abdulsalami Nasidi, pioneer Director-General, Nigeria Centre for Disease Control (NCDC) and Vice President of Reach Care Foundation, recalled how Nigeria produced an effective yellow fever vaccine which was used to control the 1986/1987 outbreak. “We could do it, we did it, and we can do it again,” he said. For this to happen, Prof. Tomori submitted that, “Self-interest needs to die, so that national interest can live.”
According to Dr Wondi Alemu, former WHO Senior Advisor, Africa and former Nigeria WHO representative, the case for immunisation is very clear. “If IA2030 is implemented according to schedule, an estimated 20 million lives in Africa will be saved.”

Dr Francis Ohanyido, Director- General, West African Institute of Public Health, stated that for advocacy to be more effective, it needs to go beyond the development space. “We need to stop preaching to the choir,” he said. Civil Society Organisations (CSOs) and the media need a seat at the table, because they can help simplify and amplify the science of vaccines. This approach will deal with poor health literacy at the grassroots level and give citizens the information that they need to hold governments at all levels accountable.

A world where everyone, everywhere, benefits
To achieve the IA2030 vision, the World Health Organization has released a framework for action, which describes how four critical and operational elements will translate strategy into implementation. These are highlighted below:
- Regional and national strategies that prioritise actions for operational planning.
- Mechanisms to ensure appropriate ownership and accountability (O&A).
- Monitoring and evaluation (M&E) frameworks to guide and monitor country implementation.
- Communication and advocacy to create the necessary messaging and reinforce the required actions by all stakeholders throughout the decade.

As of April 2022, data sourced from the CDC dashboard showed that only six African countries have a fully vaccinated rate of above 50% for COVID-19 vaccines. In Nigeria, the figure is a dismal 6%. All countries must therefore scale-up COVID-19 vaccine campaign and ensure that access is made easier where possible, as well as communications discussing the importance of COVID-19 vaccines. Collective action is needed to keep track with existing routine immunisation campaigns to ensure that children that have missed vaccinations are not left behind, while also making rebuilding of essential services, a priority.
The COVID-19 pandemic disrupted vaccination and routine immunisation activities globally. Rebuilding immunisation and strengthening of health systems at primary healthcare level will ensure that the country does not lose out on the gains made prior to the COVID-19 pandemic. Nigeria’s ten-year Strategy for Immunisation and PHC System strengthening [NSIPSS] promotes a unified approach to improve all elements of immunisation by boosting immunisation, not as a stand-alone programme, but as a key component of PHC at all levels in Nigeria. Effective childhood and adult immunisation programmes, including COVID-19, will help build resilient and sustainable primary health care systems that will be central to strengthening global health security.
On the continental level, the African Vaccine Manufacturing Initiative (AVMI) has a vision for Africa to have the capacity to produce its own vaccines for both routine and emergency purposes. The AVMI is partnering with governments, regional bodies, the private sector, academic institutions, and key opinion leaders with the aim of creating an environment on the African continent which is conducive to the emergence, development and sustainability of vaccine and biological manufacturers that meet global quality standards. There is also the Partnerships for African Vaccine Manufacturing, an initiative launched by the African Union (AU) and the Africa Centres for Disease Control and Prevention (Africa CDC) with the aim of leveraging Pan-African and global partnerships to enable Africa to manufacture 60 percent of its vaccine needs locally by 2040.
In 2020, the Central Bank of Nigeria introduced the ‘Healthcare Sector Research and Development Intervention Scheme’ (HSRDIS) as part of its policy response to the COVID-19 pandemic. The scheme is intended to boost the domestic manufacturing of critical drugs and vaccines, ensure their sustainable domestic supply, and reduce the cost of manufacturing drugs, medical devices, and vaccines in Nigeria. As at March 2021, N253.54 million worth of grants have been awarded to five researchers.
Vaccine manufacturing is a multifaceted undertaking, but it is imperative that Nigeria, and Africa continue to commit to reducing dependence on other countries for life saving vaccines and drugs.
Strengthening our health systems is critical to building resilient communities.



Immunization saves life.
#LongLifeForAll
Learning from the lessons of Covid-19 pandemic, there’s no better time than now to be prepared for future pandemics by ensuring that individual and collective efforts are required; as vaccination has proven to be a wise investment in health.